COVID-19 Vaccine Packaging and Distribution System
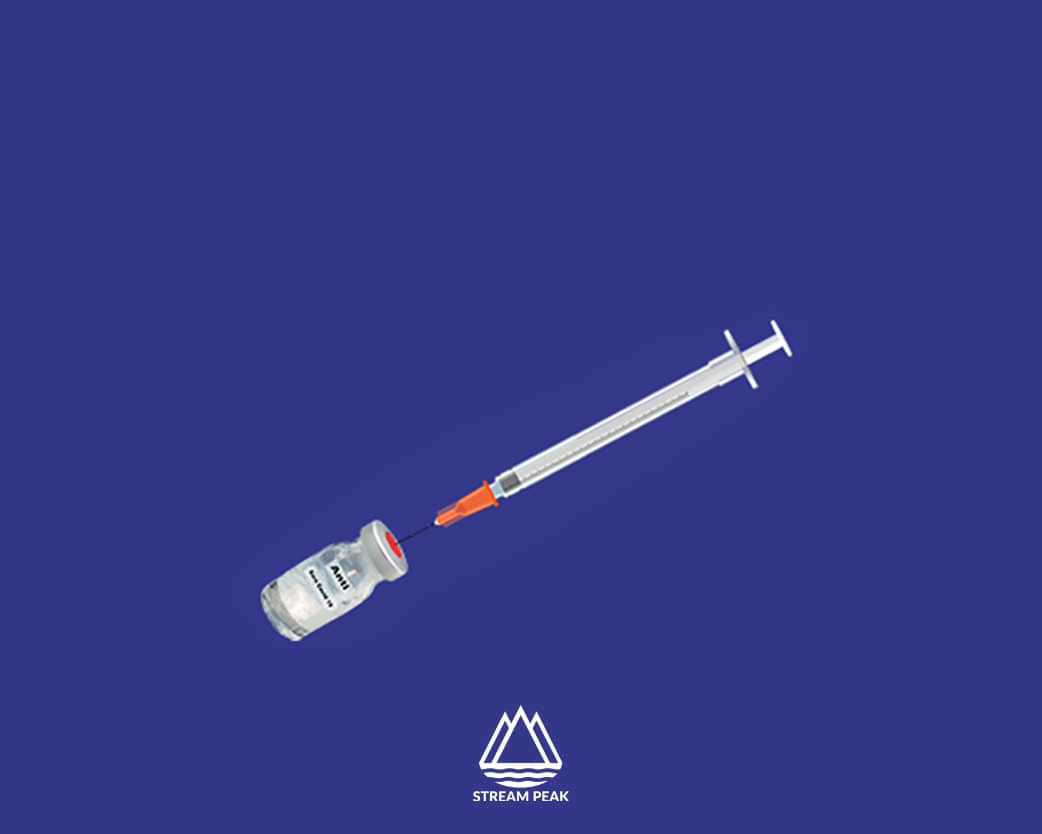
Many are already questioning shipping logistics with a COVID-19 vaccine expected to be available within the next few weeks. As the vaccines will need to be kept at a specific temperature throughout the supply chain, last-mile delivery will be the most significant challenge to get them worldwide. Truck shipments will be broken down into small units and distributed to hospitals, clinics, pharmacies, and many more. It becomes increasingly challenging to ensure temperature stability over time.
What are Temperature Indicators?
Temperature Indicators designed for last-mile delivery and point of administration use can help to ensure a smooth distribution. They help ensure that healthcare professionals receive vaccines maintained at the proper temperature during the final delivery stage before injecting them into a patient. Alternatively, Time-Temperature Indicators such as the WarmMark® will consider temperature excursions that occurred and their duration. These temperature indicators aid in protecting human health, ensure the vaccine’s effectiveness and provide a useful tool for healthcare professionals to manage inventory and avoid wasting vaccines.
How do the Indicators Help in Facilitating the Delivery Process of the Vaccines?
The vaccines are separated into many boxes, where they will be individually shipped and placed in a freezer upon arrival. This method could lead to the possibility of freezer failure, which will cause a tremendous amount of waste. Putting these temperature indicators in the inventory will help indicate which vaccines have experienced temperature excursions and can still be used.
As temperature indicators do not cost much – less than 50 cents when bought in bulk compared to $5 or more for other loggers – using these indicators is a viable solution. SpotSee®’s WarmMark® time-temperature indicator can detect a range of temperatures from -18°C (deep freeze), eight °C (refrigeration), 25°C (room temperature), and excursion times from 30 minutes to 168 hours. Besides, they are customisable to fit vaccine specifications.
Temperature labels will visibly change colours to indicate temperature excursions. For example, the WarmMark temperature labels will change from white to red to show the temperature excursions and duration. Tracking this information can be the deciding factor in administering or destroying the vaccine.
A temperature indicator would be placed every time a bulk shipment is broken down and shipped in an ideal situation. Developing such a vaccine involves many companies and research labs. According to ClinicalTrials.gov, approximately 260 vaccines are in development, and nearly 60 vaccines are in Phase III trials, which is the final step before approval for distribution to the public.
Some are expected to be approved before the end of 2020, whereas others are highly likely to be authorised throughout 2021. Monitoring vaccine storage and shipping temperatures is a global challenge that worsens with different handling temperatures due to the various vaccines.
Types of Vaccines
The vaccine comes in many forms, such as mRNA and DNA-based vaccines, protein subunit vaccines, live attenuated virus vaccines, and many more. Some are unique, where storage and temperature requirements differ from previous vaccines. For example, some mRNA vaccines require deep frozen temperatures. Vaccines developed by Pfizer and BioNTech must be stored at -70°C. When it is refrigerated at two °C- to 8°C, it lasts only ten days. Pfizer has a $1.95 billion contract with the U.S. government to supply up to 100 million doses of its vaccine.
Preparation of Vaccines
The preparation of vaccines for administration is also time-temperature sensitive. Vaccines will be supplied in multi-dose vials. Before the vaccine is administered to a patient, they have to be thawed and prepared; this leaves a window of opportunity for temperature changes. Before a vial is thawed, it must be just that enough patients will arrive in a given time frame to be able to open the vial.
Protecting vials with Time-Temperature Indicators ensures the vaccine will remain safe and effective. The WarmMark three-window temperature indicator gives additional assurance, accurately provides time-temperature data, and is cost-effective. For vaccine manufacturers and carriers, there are many factors to consider outside of arranging extra flights. As most vaccines require special handling, they must ensure that the cold chain remains intact during its peak shipping season.
 In response, UPS and Deutsche Lufthansa have plans to expand their freezer farms at airport hubs. FedEx and DHL are adding temperature monitoring systems to ensure vaccines are handled properly throughout the cold chain. McKesson, who agreed to deliver the vaccine as part of a contract signed in 2016, provided the H1N1 vaccine during the H1N1 pandemic and is supplying most flu shots.
In response, UPS and Deutsche Lufthansa have plans to expand their freezer farms at airport hubs. FedEx and DHL are adding temperature monitoring systems to ensure vaccines are handled properly throughout the cold chain. McKesson, who agreed to deliver the vaccine as part of a contract signed in 2016, provided the H1N1 vaccine during the H1N1 pandemic and is supplying most flu shots.
They plan to bring new facilities online and add employees to assemble the vaccine kits of needles, syringes, and protective equipment. Ensuring the cold chain remains intact can be challenging with such a monumental task. It is estimated that between 5% to 20% of vaccines will spoil during transportation due to improper temperature control. Good packaging could reduce the spoilage rate between 1 billion to 4 billion doses of the COVID-19 vaccine due to cold chain failures.
As temperature requirements differ drastically depending on the vaccine, each will require evidence that safe temperatures were maintained throughout the storage and shipping process. Anything can go wrong even with the best procedures and distribution getting further from reliable power and refrigeration, the evident risk that vaccines will experience temperatures that degrade their potency.
Even though many transportation hubs can ensure temperature stability, as vaccines move out of the United States, packages become smaller, leading to decreased thermal mass. This decrease will warm vaccines faster in small containers than in larger ones. Also, refrigeration facilities may be more risky as the vaccine moves from distribution centres to pharmacies or physician’s offices.
From 2014 to 2019, Australia lost nearly AUS $26 million worth of vaccines from 12,000 cold chain breaches. As a result, an estimated 747,000 vaccines were destroyed – 1.65% of all vaccines distributed in Australia. Refrigeration failures are the most common reason cited; however, some were caused as the vaccines were stored on the lowest shelf, the coldest part of the refrigerator.
A study of German physicians indicated that 16% had experienced cold chain breaches. A review of 21 refrigerators showed they were out of their set temperature ranges more than 10% of the time. The cost extends beyond unvaccinated people. The cost of the vaccine itself as companies have to destroy wasted vaccines as medical waste regardless of whether they spoil in transit or at the point of administration.
For manufacturers and healthcare providers, this leads to a loss in revenue. It also means additional manufacturing, packaging, storing, and shipping costs. Therefore, monitoring the vaccine to reduce the risk of these temperature excursions is easier and safer. Through monitoring, it acts as an early warning system, even though it will not prevent the temperature excursion. However, it will alert the users in time to minimise the impact.
Cold Chain Packaging for Vaccines
Choosing vaccine packaging should be done with possible delays in mind, as packages may be lined up and awaiting clearance. Other possible factors are changes in weather between the northern and southern hemispheres, which may place additional stress on the cold chain when the distribution point is as large as this. In every healthcare facility and pharmacy worldwide, the cost-benefit ratio changes.
For such situations, using a Data Logger for the shipment is the safest, most reliable, and cost-effective solution, with time-temperature indicators strategically placed within the cargo. With strategic placement, those receiving the vaccine can decide products in the middle have been maintained at an acceptable temperature, even if those outside have failed.
When the bulk package has been broken down into smaller quantities for individual clinics and pharmacies, Time-Temperature Indicators are the most cost-effective option. Knowing the length of an excursion allows the manufacturer to determine the safety and potency of the vaccine. Even deep-frozen vaccines thawed before administration, a temperature excursion could mean the shipment is not impaired. Still, it has to be used within a time frame, typically within hours.
These vaccines are too necessary not to safeguard. No information is available regarding whether the vaccines are susceptible to cold, but vaccines using inactivated viruses can be damaged by freezing. Furthermore, some vaccines will lose all potency when frozen. Brief heat excursions may also reduce potency but allow these vaccines to be used. Temperature Indicators indicate when the vaccine has been too hot or cold. Carriers are going to great lengths to protect the cold chain for what seems to be the largest-scale vaccination.
However, plans may go awry, refrigerated units may not be plugged in between off-loading and hands-offs, compressors fail, transportation delays, and even built-in thermometers and alarms fail. All vaccines are valuable, but the COVID-19 vaccines are too precious to risk by relying on packaging alone. Additional temperature monitors provide extra security to maintain the correct temperature or a warning where excursions occur so only safe and effective vaccines are administered.